The Mississippi State Department of Health has detected the first confirmed case of a dangerous, much more infectious variant of COVID-19, indicating that the state has limited time before it becomes the dominant strain in the region.
In a statement, MSDH confirmed that the B1.1.7 variant of COVID-19 has been detected in a resident of the state. Notably, the statement mentions that “no international travel or spread to contacts is known to have occurred,” suggesting that the variant was likely acquired through community transmission from elsewhere in the state.

Variants of SARS-CoV-2, the specific coronavirus that causes COVID-19, are the inevitable consequence of the 110 million-plus cases of confirmed COVID-19 infections worldwide.
”We are creating variants like gangbusters right now because we have so many humans infected with SARS CoV-2,” Dr. Siobhan Duffy explained to National Geographic in February. Viruses mutate as they replicate, creating new strains capable of more effectively competing for hosts.
Research from Vanderbilt University has identified coronaviruses in particular as slow to mutate, sparing humanity an even more drawn-out fight against the persistent viral foe.
A detailed study in Nature revealed that the “default” variety that became most prevalent worldwide last June is itself a mutation, one of the numerous strains of COVID-19 active globally. The study found no increased lethality from that early mutation: some of these new variants present greater dangers to public health than the original. B1.1.7 is just such a strain.
What Is B1.1.7?
B1.1.7 is a mutated form of coronavirus with significant alterations to the “spike” protein that gives the virus its crowned shape and its name. These mutations make the B1.1.7 variant of the virus much more dangerous, the Centers for Disease Control explains.
It is not completely understood how this translates into the practical infectiousness of the virus. Initially, experts including scientists at the University of São Paulo hypothesized that the mutations allowed the virus to more easily stick to the specific gateway the virus uses to infiltrate human cells.
Additionally, the Journal of Infectious Disease posits that the variant could cause a higher viral load, meaning concentration of infective matter. That would potentially mean that an infected person could transmit the virus to a healthy person over a much shorter period of time, with less interaction.
“Why is B117 more transmissible?” asked Dr. Yonatan Grad, a Harvard professor of immunology currently investigating the strain. “Some ideas include enhanced ACE-2 binding and higher or more persistent amount of virus.”
Grad’s preliminary research on B1.1.7 at the T.H. Chan School of Public Health at Harvard suggests that the variant may remain infective for significantly longer than prior strains. Examination of identified cases of B1.1.7 among NBA players and staff found a much broader range of infection duration, suggesting that for B1.1.7, the normal 14-day quarantine may prove insufficient to prevent transmission to others.
“These data offer evidence that 40 SARS-CoV-2 variant B.1.1.7 may cause longer infections with similar peak viral concentration 41 compared to non-B.1.1.7 SARS-CoV-2,” the study’s abstract states. “This extended duration may contribute to B.1.1.7 SARS42 CoV-2’s increased transmissibility.”
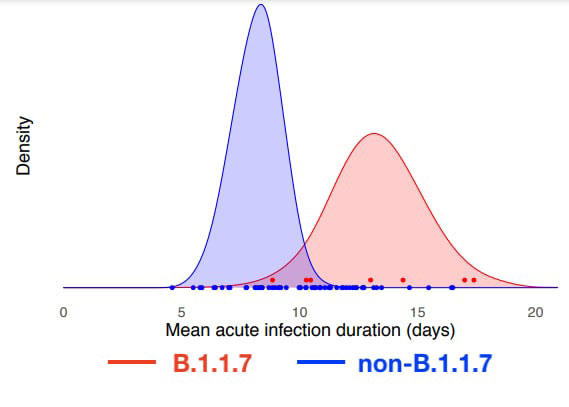
The study’s authors are quick to point out the low sample size of B1.1.7 in their research thus far. “Since there were only 7 cases of B117, we’re cautious about interpretation,” Grad explained on Twitter yesterday.
But consistent results of longer than average infections could eventually spur public-health leadership to err on the side of caution and extend the suggested quarantine time for those exposed to COVID-19.
Why is B1.1.7 Dangerous?
Regardless of the specific reason that B1.1.7 is more infectious, it is plainly a greater threat to unvaccinated populations than any strain before it.
“This virus has been working out. It’s gotten faster and more fit. And we need to fight smarter and harder to beat it,” Dr. Jeff Duchin, a Washington public-health official, told the Public Health Insider blog at the end of January.
Like any other replicating pathogen, it will eventually outcompete less aggressive variants, as it has in the U.K. where it first emerged. “Currently, the rate of infection is forbiddingly high, and I think we have to be realistic about that,” U.K. Prime Minister Boris Johnson said on Jan. 23
The best way to understand the infectivity of a virus is the “effective reproduction rate.” In the simplest possible terms, this is an estimation of how many additional infections one infection will cause. (The earlier term “r-naught” is no longer applicable with vaccinations available.)
The long sought-after herd immunity is achieved if the reproduction of the virus drops below one—if the rate is maintained, cases are in terminal decline, and the virus will eventually disappear. But the increased infectivity could push that production number up.
Experts are clear: It is not simply that more people will catch the virus. It is that measures that could have reduced the reproduction rate to a downward decline may no longer be sufficient.
“I worry we could reach a staggering death toll by the summer and fall,” Dr. Peter Hotez told USA Today on Tuesday.
There is growing—but still inconclusive—evidence that B1.1.7 is deadlier in addition to being more infectious, with British public-health officials estimating a 30% higher mortality rate from the new strain, compared to the original.
But the infectiousness is itself the deadliest element of the variant, as Dr. Adam Kucharski explained to The Atlantic last December. More cases mean more deaths, and a compounded outbreak can create the momentum necessary to harm or kill many more people than an equally infectious but individually deadlier virus.
“If the fatality rate increased by 50 percent, that would lead to 193 deaths. In contrast, a 50 percent increase in transmissibility would lead to a whopping 978 deaths in just one month,” Atlantic reporter Zeynep Tufekci explained.
Do Vaccines Work Against B1.1.7?
Both Pfizer and Moderna have released statements supporting the effectiveness of their vaccine against the B1.1.7 variant. Increasingly strong evidence from studies carried about by both companies suggests that both the Pfizer-BioNTech and Moderna vaccines available to Mississippians are effective against the B1.1.7 strain without the need for an additional booster shot.
This means that Mississippi’s effectiveness at delivering the vaccine—especially to high-risk populations like the elderly—could significantly blunt the impact of the coming spike thanks to the new variant.
Questions linger about another strain that has arrived in the United States but has yet to be sequenced in Mississippi. The CDC has reported that South Africa’s B1.351 strain is not currently believed to be more severe than the other varieties of the virus and does appear to present some resistance to antibodies and certain vaccines.
Still, Pfizer and Moderna have shown the strongest resistance to even this variant in early investigations as well.
More research is needed to determine the best course of action with regards to the new strains. What has not changed, the Mississippi State Department of Health reports, is the solution for Mississippians to protect themselves and their communities: wear a mask, avoid gatherings, and get a vaccine as soon as you qualify.










