A sharp uptick in COVID-19 testing volume last week has Mississippi public-health officials on alert for increasing transmission of the virus. State Health Officer Thomas Dobbs warned this week of a “rebound” in testing volumes, one of the early monitoring signs of an oncoming viral surge, even as new cases of COVID-19 have remained low through October and early November.
As of today, that possible surge has yet to materialize, and other data that may point to an uptick in cases—including syndromic surveillance, which monitors the appearance of COVID and COVID-like respiratory symptoms at Mississippi’s hospitals—are not yet available for the purposes of comparison.
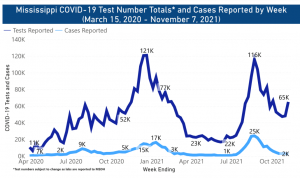
“Last year COVID rebounded right after (our) Halloween celebration,” Dobbs warned this week. In fact, mid-November was the precise moment where new cases began emerging for last winter’s surge, which peaked in early Jan. 2021. While that surge took place before widespread availability of the vaccine, it also predated the emergence of the highly infectious delta variant.
Yesterday’s seven-day average of new cases is 302—by this time last year, that average had already climbed to 947. MSDH has not released case numbers from Wednesday as of press time.
Regionally, however, the South is currently an area of low transmission, as the delta wave has passed through and washed over the rest of the nation. Currently, it is the Midwest experiencing the highest volume of new cases per capita, with an especially stiff outbreak ongoing in Alaska as well.
With nearly half of Mississippi now fully vaccinated and many thousands more having recently been infected with COVID-19, the question for the holiday season ahead is to what degree natural immunity will work together with vaccinations to keep transmission low.
Natural immunity is often a strong defense against COVID-19 reinfection, but extensive studies have called into question how long and how consistent that protection is. Expert analysis suggests that roughly one-third of COVID-19 infected patients do not develop meaningful immune response after infection.
A broad study in Emerging Infectious Diseases reported that “36% of our cohort represented serologic non-responders,” meaning that in spite of active COVID-19 infections of varying degrees of severity, patients did not develop strong immunity to the virus.
For those that do develop an antibody response to COVID-19, there is increasing evidence that this immunity is short-lived, and significantly more short-lived than antibody response from vaccines.
But the nearness of the delta wave is still a strong contender to explain why the South continues to see low transmission, even with a sluggish vaccination rate.
Some good news is still on the horizon, with promising trial results emerging from antiviral pills showing a serious reduction in hospitalizations and severe disease. Molnupiravir, an antiviral that introduces disruptions in the virus’ RNA, can disrupt and kill the virus after infection, providing another tool similar to monoclonal antibody treatment for stopping serious infections before they kill.
While the new drugs have yet to receive FDA approval, the trial results suggest that long-term management of endemic COVID-19 may employ a variety of treatments, including reactive measures that can blunt the severity of outbreaks as they occur.










